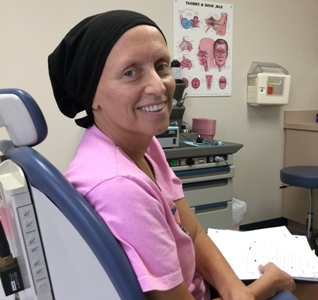
 As of now, I’m officially done with chemo. Unfortunately, that’s not because I’m cured. My oncologist has decided I’m too sick for any more. I’m afraid I have to agree.
As of now, I’m officially done with chemo. Unfortunately, that’s not because I’m cured. My oncologist has decided I’m too sick for any more. I’m afraid I have to agree.
When I first started writing this post (about a week ago now), I still had pneumonia from my first hospitalization, which was about six weeks ago. My blood counts were all off (they’ve given me platelets once and hemoglobin twice). Several nights ago, I suddenly got very short of breath. The nurse called my doctor, who ordered a blood test to see if I may have had a pulmonary embolism (a blood clot in the lungs).
It took several tests and about 2 1/2 hours for them to decide I didn’t. So I asked my nurse what she thought might be going on. She said she thought it might just be all the junk breaking up in my lungs from the pneumonia. That didn’t sound right to me. The doctor ordered breathing treatments every four hours and oxygen therapy as needed.
Over the next few days, the pain continued and the shortness of breath got worse. We knew it was being caused by swelling from a combination of throat surgeries and mucositis brought on by chemo. But nobody knew what to do about it. The nights were the worst and I’d find myself dreading them because I knew I would again be starving for air. And I was becoming confused due to a lot of medications and a shortage of oxygen to my brain.
One night, I needed to get up and use the restroom, so I called for the nurse (they had an alarm on my bed). Nobody came, so I got up on my own. I had to take my oxygen off to do it but my IV poles would reach. I went to the restroom and the breathing problem got worse. I couldn’t catch my breath and knew I was in trouble. I managed to get my pants up (whew) and staggered back to the bed to unplug my IVs. I began using every little bit of air I had left to yell for help. My alarm was going off and still nobody came. So I dragged my IV pole out to the hall in front of my room, tried to find a location where somebody might trip over me, and lay down on the floor, still yelling. Finally, somebody noticed me and people began running (because they had no choice at that point since they’d be in trouble if it looked like I fell or if somebody actually tripped over me).
I was in and out of consciousness for the rest of the night. I don’t know what all they did, but I woke up several times to find them sponging me with cold cloths, to I must have had a fever.
The next day, the cardiology team did its best to get me transferred to to oncology, which was good for them and great for me. The oncology nurses know me, and they all looked so sad to see me in such bad shape. My doctors still didn’t understand, either.
I had one nurse on the oncology unit who I knew before (she looks like my cousin, Suzette) who kept trying to connect with me. She always got down face-to-face with me and asked if I knew my name, where I was, and what day it was. The last time she asked those questions, I aced the first two, then told her it was Sunday. She said, “Julie, it’s Tuesday.” I started to argue with her, then looked at my whiteboard, which clearly said it was Tuesday.
Awhile later, the nurse came back with a doctor. They both got down face-to-face with me. The doctor said he was filling in for my oncologist. He asked if I remembered an ENT talking to me about taking some steroids. I told him I did (My oncologist and PCP had both told me no at the time). He said if I didn’t take the steroids, I’d have to have a tracheostomy. I was not going to do that! I told him I’d take the steroids.
About two hours after the nurse gave me the steroids, I called for her. She came in and smiled at me. “You have color. You’re awake,” she said. She took off the oxygen, and I’ve pretty much been awake and on room air since then. I’m also back on my home medications. I think that nurse saved my life. At least for now.
Now for the options (there aren’t many left). The plan is to go home on Hospice with the idea that we’re not giving up; more like taking a break. I’m having a PET scan first to see if I have any tumors besides the one in my liver. If not, I’ll have it surgically removed (ablated). As long as the sodium stays in check, we do nothing except for whatever routine services Hospice provides (like pain management without drugging me into oblivion, routine labs to check my sodium). Last time it took almost a year for another tumor to come back. So we’ll see what happens this time.
If there were indications of another tumor later on, we could see if it could again be ablated. If so, we’d again do it and then do nothing until the next one came around.
At one or more points throughout this process if we needed to switch from Hospice care services to palliative care services, it could be done pretty easily since the organization we’ll be working with does both.
If we get to a point (hopefully several years down the road) where the surgical ablations no longer work, we’ll move to a clinical trial. The drug is the one you’ve heard being advertised for non small-cell lung cancer (Opdivo.) It’s not yet been approved for small-cell cancer, but hopefully it will be or I’ll get into a clinical trial when the time comes. You can actually get the drug outside a clinical trial, but it’s a lot harder to get insurance to pay for it. People are doing it anyway, which may help get it approved faster it if appears to be working.
That’s it for now. Thanks for reading my blog. If you’d like to help me with my battle with cancer, please go to https://www.youcaring.com/julie-mears-henry-495041.
6 Responses to “Running out of options (Sort of)”
Sorry, the comment form is closed at this time.
You are such an amazing human being. By documenting your experience you are helping others in similar situations, while never losing your sense of humor.
I will pray for you to Buddha, the Virgin of Guadalupe and Obatalá, just to make sure you are fully covered.
Un abrazo,
Mireya
You are amazing. My prayers are with you ever day and more.
Yes, you are definitely amazing Jules! I am speechless! Thinking of you and big, big hugs to you!
Love you my friend.
Thanks! I appreciate the coverage.
When I meditate, my deep healing breaths are for you. I have asked other friends to pray for you also, I figure the more god hears from all of us the better. You know safety in numbers kind of thing.
I am glad you are taking a break from all this and I pray that it will works in your favor. I think you have been one tough cookie through all this. But I have always know you can be one tough cookie for years, love you. Oh and glad you get to go home, you know that saying theres no place like home.
You are such an inspiration, Julie. I pray that you regain strength and faith enough to rebound and stand on your own to fight this. You seem to have a lot of people standing with you. Please count me in as well!